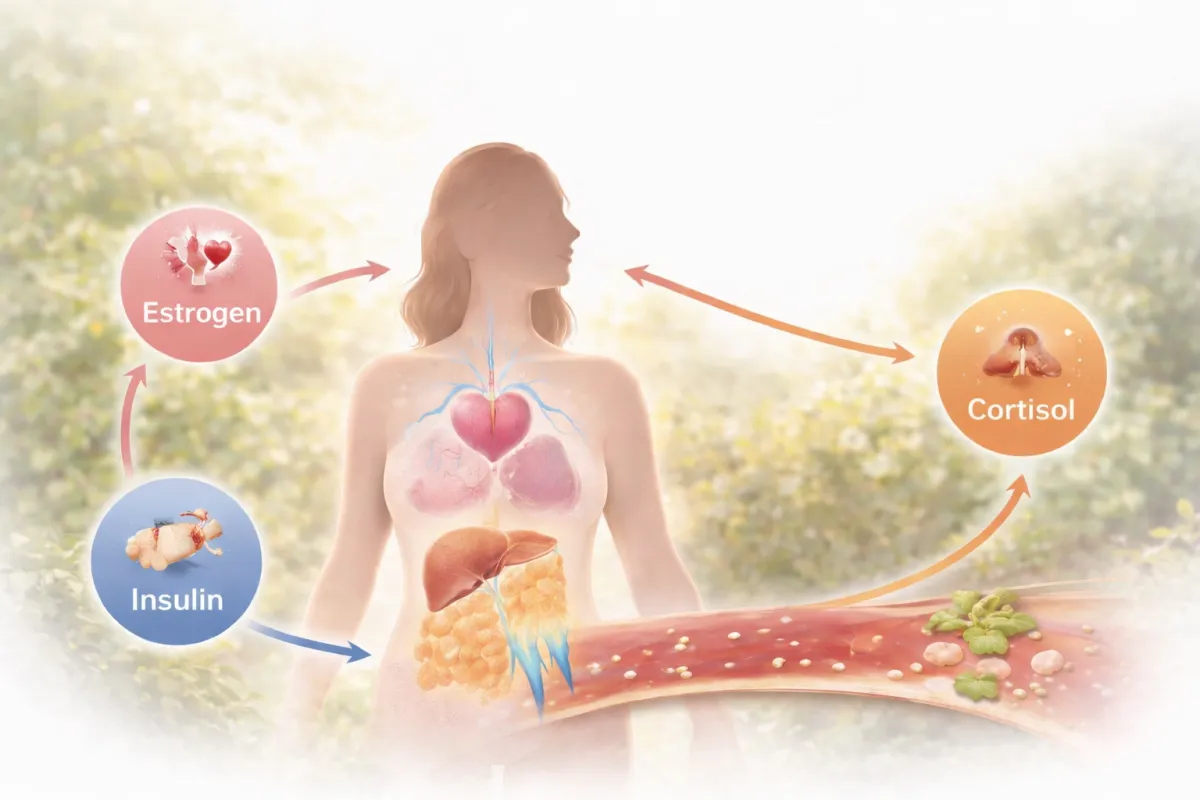
Why Midlife Hormones Change Cholesterol, Blood Sugar, and Weight
Midlife Hormones, Cholesterol, and Metabolism: Why Your Body Feels Different After 40
Many women notice changes in their health during midlife that feel sudden and unexplained. Cholesterol levels rise. Weight becomes harder to manage. Energy drops. Blood sugar shifts. And often, this happens even when diet and exercise have not changed.
These changes are not a failure of discipline or effort. They are driven by normal physiologic shifts in hormones that begin years before menopause.
Understanding how hormones influence cholesterol, insulin, and metabolism is essential to making sense of what is happening in the body during this stage of life.
The Midlife Hormone Shift
Perimenopause can begin in the late 30s or early 40s, long before periods stop. During this time, estrogen and progesterone fluctuate unpredictably before gradually declining.
These hormones do far more than regulate the menstrual cycle. They play protective roles in metabolic health, insulin sensitivity, lipid processing, inflammation, and energy regulation. When hormone signaling becomes inconsistent, downstream metabolic changes often follow.
This transition is physiologic, not pathological. But without context, it is often misunderstood.
Hormones and Cholesterol
Estrogen plays a key role in how the body processes cholesterol. It supports healthy HDL levels, helps clear LDL from circulation, and protects the lining of blood vessels.
As estrogen fluctuates and then declines, these protective effects lessen. Many women see:
Rising LDL cholesterol.
Changes in cholesterol particle size and number.
Increased inflammatory signaling.
Importantly, these shifts can occur even in women who eat well, exercise regularly, and have never had cholesterol issues before. Cholesterol changes in midlife are often a signal of hormonal transition, not simply diet-related risk.
Hormones and Insulin Sensitivity
Estrogen also influences how cells respond to insulin. When estrogen levels decline or fluctuate, insulin sensitivity can decrease, meaning the body needs more insulin to manage blood sugar effectively.
Over time, this can contribute to:
Elevated fasting glucose or insulin.
Increased fat storage, especially around the abdomen.
Energy crashes and cravings.
Difficulty losing weight despite calorie restriction.
This is why many women feel as though their metabolism has suddenly slowed. In reality, their metabolic signaling has changed.
The Role of Stress and Muscle Loss
Midlife is often accompanied by increased life stress, disrupted sleep, and loss of muscle mass. These factors further affect insulin sensitivity and metabolic efficiency.
Chronic stress raises cortisol, which can worsen blood sugar control and promote fat storage. Loss of muscle reduces the body’s ability to use glucose efficiently. Together, these shifts compound the hormonal changes already underway.
This is why approaches that rely solely on eating less and exercising more often fail during this stage.
Why Everything Feels Connected
Hormones, cholesterol, insulin, and metabolism do not function independently. They operate as an integrated system. When one part changes, the others respond.
Midlife metabolic changes are rarely about a single hormone or lab value. They reflect a broader physiologic transition that deserves context, education, and individualized support.
What Actually Helps
Supporting health during midlife starts with understanding what the body is doing and why. Effective strategies focus on:
Preserving muscle mass.
Supporting insulin sensitivity.
Managing stress and sleep.
Interpreting labs through a hormonal lens.
Avoiding chronic under-eating that worsens metabolic adaptation.
Midlife is not a decline. It is a transition. With the right approach, it can be a period of clarity, strength, and renewed health rather than frustration.
